By Hannah McNeish
 NAIROBI, KENYA: Having clothes ruined by ink and inhaling chemicals for hours in the hospital darkroom used to bother Margaret Njuwe and other radiographers at East Africa’s largest referral hospital in Kenya’s capital Nairobi.
NAIROBI, KENYA: Having clothes ruined by ink and inhaling chemicals for hours in the hospital darkroom used to bother Margaret Njuwe and other radiographers at East Africa’s largest referral hospital in Kenya’s capital Nairobi.
But when ink runs rendered X-rays unusable or mammograms came out too soft to see suspected lumps, Njuwe’s heart would sink as she climbed Kenyatta National Hospital’s (KNH) stairs to the radiology department’s constantly packed waiting room.
“Patients would wait for hours, and then maybe when you go to the darkroom you have to repeat [the scan] and call the patient back and it might take another day”
“Patients would wait for hours, and then maybe when you go to the darkroom you have to repeat [the scan] and call the patient back and it might take another day,” she said.
Some patients in the 2,000-bed hospital would come back. Others, especially referrals from other centers, would disappear, regardless of how sick they were.
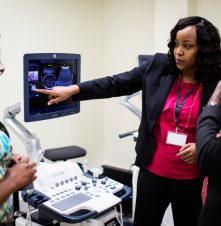
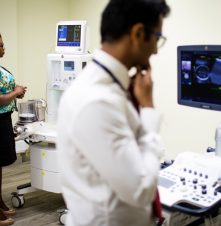
But for the past three months, KNH staff have switched from analogue to digital machines and been able to scan and sometimes diagnose patients within minutes.
“It has reduced those delays. Patients can be referred instantly, because you can take an image, you print it instantly and the patient can take it with them to the referring doctor instantly,” said radiographer Clifford Ike.
In total, 98 hospitals in Kenya will benefit from a program being led by the Ministry of Health to modernize core healthcare services at key government facilities across the country. It is the first Government-led program of its kind in Kenya — and one of the largest undertaken to date in Africa to support sustainable healthcare development.
Selected by the Ministry as the technology provider for the radiology modernization tranche of the Kenya mega tender – GE, a committed partner in the development of healthcare in Africa, is providing a comprehensive program that includes the installation of 585 new machines across all 47 counties – and over the next seven years will provide the medical staff using them training and technical support to ensure the optimal operation of the equipment.
After years of studying health models, “without a doubt the ones that have proven to be successful when serving populations is collaboration between the public and private sectors,” said Terri Bresenham, CEO of GE Healthcare’s Sustainable Healthcare Solutions business.
“As a company what we do know how to do well is set up a structure and capital investment.”
GE’s plan differs from “this huge capital investment up front and then nothing left for maintenance and for training,” she added.
KNH’s basement has just some of the many abandoned or broken down machines that litter health centers nationwide as parts or know-how to use them were missing.
The first 44 hospitals to go digital – one of Kenya’s healthcare focuses for its 2030 Vision plan – using the new machines increased monthly examinations from 1,500 to over 28,800.
At Mbagathi hospital in downtown Nairobi, staff using one of GE’s temporary x-ray machines until their equipment is installed is now doing up to 100 scans a day, almost double what the old machine did.
“They are doing it quickly-just some minutes”, said Frida Ngute, whose baby Agnes has had chest problems for three months.
Mbgaathi Hospital Radiographer Irene Githinji is looking forward to switching from expensive film rolls to digital machines for ultrasound, x-ray and surgery, especially as the hospital is next to Kibera – a slum where millions of people live.
“We are hoping that eventually it will help us make it even cheaper for them,” she said.
To ensure quality, standardized and continued training for Kenyan health workers and as part of GE’s plan to train 10,000 by 2020, on June 16, GE Healthcare’s CEO John Flannery opened its “first dedicated center in Africa for training on technology”.
“Demand for quality healthcare is increasing”, said Cleopa Mailu, Kenya’s Cabinet Secretary for the Ministry of Health, at the inauguration of the center in Nairobi’s Karen neighborhood.
“This dedicated training center will bring people together”
“The GE Healthcare Training Center will play a critical role in supporting the capacity development of biomedical engineers, radiologists and technicians, helping to reduce the skills gap, improve job prospects and build a solid national healthcare system,” he added.
“This dedicated training center will bring people together”, help build networks of specialists and bridges with health workers in different tiers or sectors of the health care system, said Bresenham.
Many communicable diseases like HIV, malaria and TB are still set up and funded separately, whereas more needs to be done to build “a better, more robust primary care system,” said Bresenham.
At KNH’s radiology department, where Njuwe scans people who have been in road traffic accidents, people suspected of having pneumonia and surgical patients, the system is already more joined up.
Ike says that the scanners have improved diagnosis times as they are “easier to work with” and have a greater range of exposures.
“People are really appreciating these machines”, he said.
Hannah McNeish is a freelance journalist based in East, Central and Southern Africa and wrote this story on assignment for The Pulse.
Más información: Out of the Darkroom, Into the Light: Going Digital in Nairobi